Understanding IVF success rates in San Diego requires more than scanning percentages on a website. For intended parents navigating fertility treatment, success is nuanced, biologically individualized, and increasingly influenced by technological precision. One of the most discussed advancements today is AI-assisted embryo selection. But does it truly make a difference?
What Do IVF Success Rates Really Mean?
IVF success rates are commonly presented as percentages, yet the terminology behind these numbers matters.
A pregnancy rate reflects how often a positive pregnancy test occurs after embryo transfer. A live birth rate, however, measures the percentage of cycles that result in a baby being born. Clinically, the live birth rate is the most meaningful benchmark.
Success rates are also highly age-dependent. Patients under 35 generally experience higher outcomes compared to those over 40, largely due to differences in ovarian reserve and egg quality.
“Success rates should never be interpreted in isolation,” explains Dr. Minoos Hosseinzadeh. “Each patient brings a unique biological profile, and our goal is to optimize every variable within our control.”
This reinforces an essential point. IVF success rates are directional indicators, not guarantees.
What Actually Impacts IVF Success Rates
Several interconnected factors influence IVF outcomes:
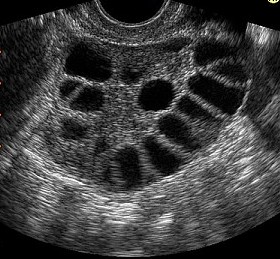
- Age and ovarian reserve
- Egg and sperm quality
- Uterine receptivity and endometrial health
- Laboratory environment and medical protocols
- Embryo selection methodology
Among these, embryo selection is often underestimated. While biology sets the foundation, selecting the most viable embryo plays a decisive role in whether implantation occurs.
How Embryos Are Traditionally Selected
Historically, embryo selection has relied on morphology-based grading.
Embryologists evaluate embryos at specific time points, assessing characteristics such as cell symmetry, fragmentation, and developmental stage. These observations are used to assign a quality score.
However, this approach has limitations:
- Evaluations occur at fixed intervals, not continuously
- Subtle developmental dynamics may be missed
- Interpretation depends on human judgment
Two experienced embryologists may review the same embryo and arrive at slightly different conclusions. This variability is not due to lack of expertise, but rather the inherent subjectivity of visual assessment.
The Challenge of Subjectivity in Embryo Grading
Human expertise remains central to IVF. Yet even the most skilled professionals operate within biological and observational constraints.
Embryo development is a dynamic process. Static snapshots cannot fully capture the intricacies of cell division timing, synchronicity, and developmental pacing.
“Embryology has always required a high level of interpretation,” says Dr. Hosseinzadeh. “What we are now able to do is complement that expertise with objective data that was previously inaccessible.”
This introduces a critical shift. Moving from subjective interpretation toward data-informed evaluation.
How AI-Assisted Embryo Selection Works
Time-Lapse Embryo Monitoring
Time-lapse technology, often referred to as EmbryoScope, continuously captures images of embryo development without removing them from the incubator.
This provides:
- Continuous monitoring rather than intermittent observation
- Thousands of developmental data points
- A stable, undisturbed culture environment
Instead of relying on isolated snapshots, embryologists gain access to a complete developmental timeline.
Chloe AI and Pattern Recognition
Chloe AI builds upon this data-rich environment by analyzing morphokinetic patterns.
It evaluates:
- Timing of cell divisions
- Developmental milestones
- Subtle deviations linked to implantation potential
Through machine learning, Chloe AI identifies patterns associated with higher developmental competence. It processes significantly more data than human observation alone, offering an additional analytical layer.
Objectivity in Embryo Selection and Why It Matters
The introduction of AI into embryology is not about replacing clinicians. It is about enhancing decision-making.
AI contributes to:
- Standardization across embryo evaluations
- Reduced inter-observer variability
- Increased consistency across cases
Chloe AI does not replace embryologists. It augments their expertise by providing objective insights that complement visual grading.
This shift toward consistency is particularly valuable in high-stakes decisions where small differences can influence outcomes.
Precision IVF at Fertility Institute of San Diego
Fertility Institute of San Diego is currently the only clinic in San Diego that includes AI-assisted EmbryoScope technology with Chloe AI as part of every IVF cycle.
Importantly, this is not an optional add-on.
It is integrated into a precision IVF framework that combines:
- Advanced laboratory technology
- Individualized treatment protocols
- Data-driven embryo selection
“Our approach is to reduce uncertainty wherever possible,” notes Dr. Hosseinzadeh. “Precision IVF allows us to align clinical expertise with advanced analytics for more informed decision-making.”
Does AI-Assisted Embryo Selection Improve IVF Success Rates?
AI-assisted embryo selection does not guarantee success. However, it can improve the quality of clinical decisions.
Potential advantages include:
- Greater confidence in embryo prioritization
- Improved consistency in selection criteria
- Support for single embryo transfer strategies
- Reduction in unnecessary transfers
Rather than promising higher success rates, AI enhances the selection process itself. This distinction is critical for maintaining clinical transparency and patient trust.
Who Benefits Most From AI-Assisted IVF?
- Patients over 35
- Individuals with limited embryo numbers
- Patients with previous IVF failure
- Donor egg IVF cycles
- Surrogacy journeys
- International patients coordinating treatment remotely
For these patients, every embryo carries heightened importance, making selection accuracy even more consequential.
IVF Success Is Not One Factor, It’s a System
IVF outcomes are the result of a complex system.
Success depends on the interplay between:
- Laboratory quality
- Physician expertise
- Patient-specific biology
- Treatment customization
AI is one component within this ecosystem. It strengthens one of the most critical steps, but it does not function in isolation.
Choosing an IVF Clinic in San Diego, What to Look For
When evaluating a fertility clinic in San Diego, consider the following:
- Laboratory technology and consistency
- Experience of the embryology team
- Degree of personalization in treatment plans
- Level of communication from their physician
A clinic’s philosophy matters as much as its statistics. Look for a balance of innovation, experience, and individualized care.
FAQ
Does AI improve IVF success rates?
AI does not guarantee higher success rates. It improves the accuracy and consistency of embryo selection, which can support better clinical decisions.
What affects IVF success rates the most?
Age, egg quality, sperm health, uterine environment, and embryo selection all play significant roles.
How are embryos selected in IVF?
Traditionally through visual grading. Advanced clinics now use time-lapse imaging and AI to enhance selection.
Is embryo grading subjective?
Yes. Even experienced embryologists may interpret embryos slightly differently based on visual assessment.
What is Chloe AI in IVF?
Chloe AI is a machine learning system that analyzes embryo development patterns to assist in selection decisions.
Is AI-assisted IVF available in San Diego?
Yes, but availability is limited. Fertility Institute of San Diego integrates this technology into all IVF cycles.
Should I choose a clinic based on success rates alone?
No. Success rates should be evaluated alongside technology, expertise, and personalized care.