For many patients navigating IVF over 35, the conversation shifts from abundance to precision. The clinical reality is not about producing more embryos, but about selecting the right embryo with the highest potential for implantation. This distinction becomes especially critical in cases of diminished ovarian reserve IVF, where each embryo carries significant weight in the outcome.
At Fertility Institute of San Diego, this philosophy is embedded into what is referred to as precision IVF, where advanced laboratory technology and AI embryo selection converge to optimize decision-making.
Why Fertility Changes After 35
Fertility decline is not abrupt, but it becomes clinically relevant after age 35 due to several interrelated biological factors:
- Egg quality decline resulting from increased chromosomal instability
- Reduced ovarian reserve, often reflected in lower AMH levels
- Higher rates of aneuploid embryos
- Greater variability in IVF success rates over 35
“After 35, we are not just working with fewer eggs, but with a higher proportion of embryos that may not develop normally. That shifts our focus toward selection rather than volume.”
Dr. Minoos Hosseinzadeh
Understanding Diminished Ovarian Reserve (DOR)
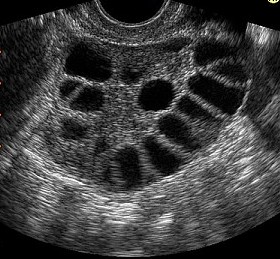
Diminished ovarian reserve IVF refers to a condition where the ovaries yield fewer eggs than expected for age. It is typically evaluated through:
- AMH levels (Anti-Müllerian Hormone)
- Antral follicle count (AFC) via ultrasound
In practical terms:
- Fewer eggs retrieved during stimulation
- Fewer embryos available for transfer
- Reduced margin for trial-and-error approaches
This leads to a pivotal shift: when embryo numbers are limited, selecting the best embryo becomes exponentially more important.
The Real Challenge in IVF Over 35: Quality, Not Quantity
Patients often ask how many embryos are needed for success in IVF over 35. The more relevant question is: how do we identify the embryo with the highest implantation potential?
- Not all embryos are viable
- Fewer embryos mean fewer opportunities
- Each transfer carries greater clinical significance
This is particularly true in IVF with few embryos strategy, where inefficient selection can lead to unnecessary transfers and emotional fatigue.
How Embryos Are Traditionally Selected
Historically, embryo selection has relied on:
- Morphological grading at fixed time points
- Visual assessment of symmetry, fragmentation, and development
- Embryologist interpretation
While effective, this approach has limitations:
- Snapshots rather than continuous observation
- Variability between embryologists
- Limited data inputs
Why Subjectivity Matters More in DOR Cases
In cycles with many embryos, minor differences in grading may not significantly impact outcomes. However, in IVF with diminished ovarian reserve, the margin for error narrows.
- One embryo may determine the cycle outcome
- Small interpretative differences become clinically significant
- Consistency becomes essential
“When a patient has only two or three embryos, every decision carries weight. Reducing subjectivity in that moment becomes incredibly valuable.”
Dr. Minoos Hosseinzadeh
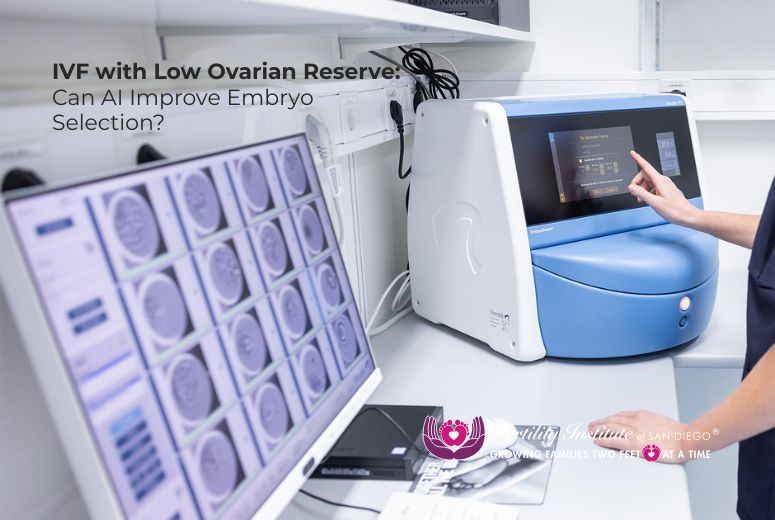
How AI-Assisted Embryo Selection Works
Time-Lapse Monitoring
Advanced systems such as EmbryoScope allow:
- Continuous imaging of embryo development
- Stable culture conditions without disturbance
- Full morphokinetic tracking
This provides a dynamic view of blastocyst development, rather than isolated snapshots.
Chloe AI and Data-Driven Analysis
AI embryo selection platforms such as Chloe AI analyze:
- Timing of cell divisions
- Developmental patterns associated with implantation
- Subtle deviations not visible to the human eye
This results in an additional layer of objective scoring that complements embryologist expertise.
Objectivity in Embryo Selection: Why It Matters After 35
AI embryo selection does not replace clinical judgment. It enhances it.
- Reduced inter-observer variability
- Increased consistency across cases
- Utilization of large datasets beyond human capacity
AI helps prioritize embryos based on measurable developmental competence, particularly relevant in embryo selection with low egg count scenarios.
Precision IVF at Fertility Institute of San Diego
Fertility Institute of San Diego is currently the only clinic in San Diego that includes AI-assisted EmbryoScope technology with Chloe AI as part of every IVF cycle.
This integration is:
- Standard, not optional
- Embedded into laboratory workflow
- Especially valuable for:
- Advanced maternal age IVF options
- DOR patients
- Limited embryo cohorts
Can AI Improve Implantation Rates?
The question “can AI improve IVF outcomes” requires a nuanced answer.
AI embryo selection can:
- Improve confidence in selecting embryos
- Support prioritization of embryos with higher developmental potential
- Assist in single embryo transfer strategies
However:
- It does not guarantee implantation
- Outcomes still depend on:
- Embryo genetics
- Uterine receptivity
- Overall patient health
“AI helps us make more informed decisions, but IVF success remains multifactorial. It is about optimizing each step, not promising outcomes.”
Dr. Minoos Hosseinzadeh
When to Consider Alternative Options
For some patients, especially with IVF success with low ovarian reserve, additional strategies may be considered:
- Embryo banking across multiple cycles
- PGT embryo testing for chromosomal screening
- Donor egg IVF as an alternative pathway
IVF Over 35 Is About Strategy, Not Speed
- Individualized protocols
- Efficient embryo selection
- Minimizing unnecessary transfers
Choosing the Right IVF Clinic for DOR Patients
- Laboratory technology and standards
- Experience with IVF over 35 patients
- Embryo selection methodology
- Transparency in outcomes and expectations
FAQs
Can IVF work after 35?
Yes. IVF success rates over 35 vary, but outcomes can be optimized with personalized protocols and advanced embryo selection.
What is diminished ovarian reserve?
It refers to reduced egg quantity, often measured through AMH levels and AFC.
How many embryos do you need for IVF success?
There is no fixed number. The focus is on selecting the embryo with the highest implantation potential.
Does AI improve embryo selection?
AI embryo selection enhances objectivity and consistency but does not replace clinical expertise.
Can AI increase implantation rates?
It can improve selection accuracy, which may support implantation, but it does not guarantee success.
Is IVF worth it with low ovarian reserve?
Yes, with the right strategy and expectations, many patients achieve success.
Should I consider donor eggs after 35?
This depends on ovarian reserve, prior outcomes, and personal preferences.
Final Step
If you’re ready to start your fertility journey, please book a complimentary virtual consultation with Dr. Hosseinzadeh to go over your options and next steps.