When you are told you have low ovarian reserve, the conversation around IVF changes. It becomes less about volume and more about precision. Fewer eggs. Fewer embryos. Higher stakes with every decision.
For patients navigating low ovarian reserve IVF or diminished ovarian reserve IVF, the question is no longer simply “Will IVF work?” It becomes more nuanced: How do we make the best possible decision with the embryos we have?
At this stage, embryo selection becomes the fulcrum of success. And increasingly, AI embryo selection is playing a role in making that decision more informed and consistent.
What Does Low Ovarian Reserve Mean?
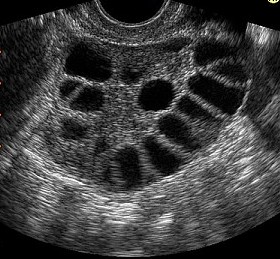
Low ovarian reserve refers to a reduced quantity of eggs remaining in the ovaries.
It is typically assessed using:
- AMH levels
- Antral follicle count
- Age-related ovarian decline
While diminished ovarian reserve IVF patients may still conceive, the IVF strategy must adapt.
You may retrieve:
- Fewer eggs per cycle
- Fewer embryos reaching blastocyst stage
“Low ovarian reserve does not mean no chance. It means we must be far more strategic with every step.”
Dr. Minoos Hosseinzadeh
The Reality of IVF with Low Ovarian Reserve
Patients undergoing IVF with few eggs retrieved often experience:
- Limited embryo numbers
- Fewer transfer opportunities
- Greater emotional and financial weight per cycle
The critical shift is this:
The challenge is not just creating embryos. It is selecting the right one.
Quality Over Quantity — The Core IVF Strategy in DOR
In diminished ovarian reserve IVF, quality becomes the central metric.
- Not all embryos are viable
- Some embryos may arrest during development
- Others may not implant
This creates a scenario where embryo quality vs quantity IVF becomes a defining principle.
Each embryo transfer is not just a step. It is a decision with amplified consequences.
How Embryos Are Traditionally Selected
Historically, embryo selection has relied on:
- Morphology grading
- Visual assessment at fixed time points
- Embryologist interpretation
While effective, this method introduces variability.
Two embryologists may evaluate the same embryo slightly differently. In cases with many embryos, this variability may not significantly affect outcomes.
But in embryo selection with low egg count, even small differences matter.
Why Subjectivity Becomes a Bigger Problem in DOR
In high-response IVF cycles:
- More embryos create a buffer
- Selection variability is diluted
In low ovarian reserve cases:
- Every embryo carries significant importance
- Selection variability has greater impact
When you only have one or two embryos, the margin for interpretive error becomes much smaller.
This is where objectivity becomes valuable.
How AI-Assisted Embryo Selection Works
Time-Lapse Monitoring
Modern IVF labs use time-lapse systems such as EmbryoScope technology:
- Continuous imaging of embryo development
- No need to remove embryos from incubation
- Full developmental timeline captured
This provides a far more detailed dataset than traditional snapshots.
Chloe AI and Data-Driven Insights
AI platforms like Chloe analyze morphokinetics:
- Cell division timing
- Developmental patterns
- Subtle growth irregularities
Instead of relying solely on visual grading, AI embryo selection introduces:
- Pattern recognition across thousands of embryos
- Consistent scoring support
- Additional decision layers for embryologists
“AI does not replace the embryologist. It augments our ability to interpret complex developmental patterns with greater consistency.”
Dr. Hosseinzadeh
Objectivity in Embryo Selection — Why It Matters Most in DOR
In IVF strategy for diminished ovarian reserve, objectivity is not a luxury. It is a necessity.
AI-assisted systems help:
- Reduce inter-observer variability
- Standardize embryo assessment
- Utilize more data than the human eye alone
This is particularly relevant in:
- Advanced maternal age and DOR IVF
- IVF implantation with few embryos
- Cases with only one viable blastocyst
The goal is not perfection. It is improved decision quality.
Precision IVF at Fertility Institute of San Diego
Fertility Institute of San Diego is currently the only clinic in San Diego that includes AI-assisted EmbryoScope technology with Chloe AI as part of every IVF cycle.
This approach is integrated, not optional.
Precision IVF at FISD focuses on:
- Data-informed embryo selection
- Consistent laboratory standards
- Personalized patient strategies
This is particularly relevant for:
- Low ovarian reserve IVF patients
- Patients with previous failed cycles
- Those with limited embryo availability
Can AI Improve Outcomes in Low Ovarian Reserve?
| AI Can | AI Cannot |
|---|---|
| Improve embryo prioritization | Increase egg count |
| Support single embryo transfer decisions | Reverse ovarian aging |
| Reduce unnecessary transfers | Guarantee pregnancy |
The value lies in improving how decisions are made, not promising outcomes.
When Additional Strategies May Be Considered
For patients with IVF with few eggs retrieved, complementary strategies may include:
- Multiple retrieval cycles
- Embryo banking
- PGT embryo testing
- Donor egg IVF
Each option is personalized.
“We tailor the plan based on ovarian response, age, and patient goals. There is no one-size-fits-all pathway.”
Dr. Hosseinzadeh
IVF with Low Ovarian Reserve Is About Efficiency
- Maximizing each cycle
- Reducing uncertainty
- Leveraging data-driven tools
The best IVF approach for DOR patients, the emphasis is not on doing more. It is on doing better with what is available.
Choosing the Right IVF Clinic for DOR
When selecting a fertility clinic San Diego, consider:
- Laboratory technology and standards
- Embryo selection methodology
- Experience with low-response patients
- Transparency in treatment planning
Clinics offering precision IVF and AI-assisted tools may provide a more structured and consistent approach to embryo selection.
FAQs
Can IVF work with low ovarian reserve?
Yes, but success depends on egg quality, age, and strategy. IVF is often tailored to maximize limited embryos.
What is diminished ovarian reserve?
It refers to reduced egg quantity and sometimes quality, often measured through AMH levels and follicle count.
How many eggs are needed for IVF success?
There is no fixed number. Some patients succeed with few embryos, especially when selection is optimized.
Does AI help embryo selection?
Yes, AI provides additional data and consistency, supporting embryologists in selecting embryos.
Can AI improve IVF success rates?
AI improves decision-making quality. It may contribute to better outcomes but does not guarantee success.
Is IVF worth it with low AMH?
It can be, especially with a personalized strategy and advanced lab support.
Should I consider donor eggs with DOR?
This depends on individual goals, age, and response to IVF cycles.
If You’re Ready to Take the Next Step
If you’re navigating low ovarian reserve IVF and want a strategy tailored to your situation, you can book a complimentary virtual consultation with Dr. Hosseinzadeh to explore your options and next steps.